What Is Fascia and How to Keep It Healthy
- Courtney Bargar, LMT
- Apr 4
- 5 min read
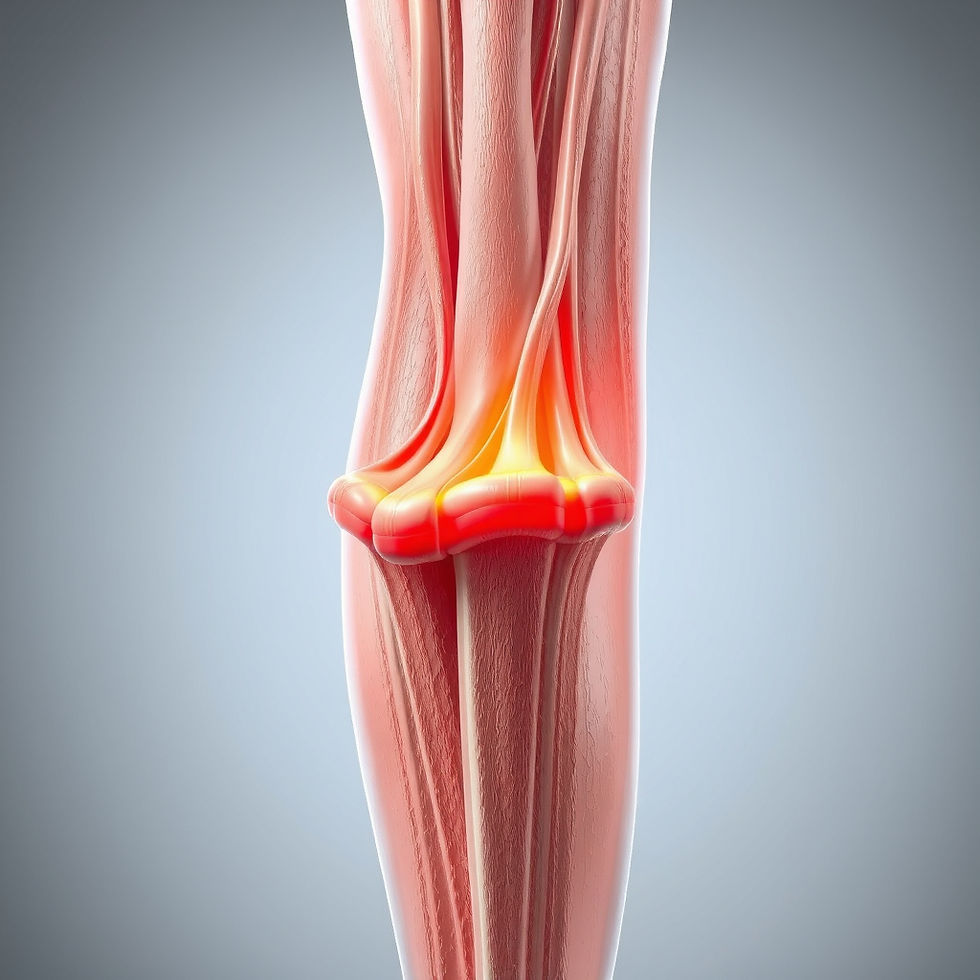
Fascia is a thin, web‑like layer of connective tissue that wraps around every structure in your body—muscles, bones, nerves, blood vessels, and organs—like an internal “body suit.” It’s made up of multiple layers of soft, stringy tissue that are flexible and designed to move with you, not lock you down. Think of it as the body’s continuous 3‑D support network, connecting everything from head to toe so your parts can glide and slide smoothly against one another.
What fascia does in your body
Fascia plays several key roles beyond just “holding organs in place.” It:
Supports and stabilizes muscles, joints, and organs, giving your body form and strength.
Allows smooth movement by creating a slippery interface so muscles and tissues can glide without friction or tearing.
Transmits force so when one muscle contracts, tension and movement can spread through the fascial network, helping your whole body coordinate.
Is highly sensitive, housing more nerve endings than muscle and even rivaling skin in how much it “feels,” so tight or irritated fascia often shows up as pain or stiffness.
What fascia is made of
Fascia is largely built from collagen fibers, the same strong, flexible protein found in tendons and ligaments. These fibers give fascia its tensile strength and help it resist tension. Mixed in with collagen are small amounts of elastin, which adds stretch and recoil, plus a gel‑like ground substance rich in hyaluronan and other glycosaminoglycans that hold water and keep the tissue slippery and hydrated. This fluid “ground substance” is what lets the fascial layers slide over one another when you move—if it dries out or becomes inflamed, movement can turn sticky and painful.
What happens when nutrition is out of balance
When your body is chronically under‑nourished or flooded with pro‑inflammatory foods, fascia loses its resilience and mobility.
Diets high in sugar, processed oils, refined carbs, and additives promote systemic inflammation, which can make fascia stiffer, thicker, and more prone to adhesions.
Inadequate protein, vitamin C, and collagen precursors (like glycine, proline, and copper) impair the repair and remodeling of collagen, leading to fascia that is weaker, more brittle, or slow to heal.
Poor hydration and gut imbalance reduce the water content of the ground substance and limit absorption of key nutrients, which can show up as increased stiffness, trigger points, and myofascial pain.
From a clinical perspective, supporting with anti‑inflammatory, whole‑food patterns—rich in colorful plants, omega‑3s, clean protein, and plenty of fluids—goes a long way toward helping fascia stay supple and responsive.
Fascia in complex neuroconnective‑tissue disorders
Ehlers‑Danlos Syndrome (EDS) and fascia
In Ehlers‑Danlos Syndrome, especially the hypermobile type (hEDS), the problem is not just “loose joints” but a fundamental change in the connective‑tissue matrix, including fascia.
Collagen defects mean fascia can be abnormally loose or paradoxically thicken in some areas, forming dense, restricted bands that pull on nerves, vessels, and muscles.
Altered hyaluronan and extracellular matrix can cause fascial layers to “stick” together, reducing glide and creating chronic myofascial pain, stiffness, and joint instability.
Trigger points and fascial densification are common, so individuals may feel deep, diffuse aching, burning, or “band‑like” tension that does not track neatly to one muscle group.
For those with EDS or Hypermobility Spectrum Disorders, the goal is often not aggressive stretching but gentle, proprioceptive work and Assisted Dynamic stretching that restores balance, supports joint stability, and re‑educates the nervous system without over‑stretching already fragile tissue.
Multiple Sclerosis and fascia
Multiple Sclerosis is a neuroimmune condition that primarily affects the central nervous system, but it can profoundly influence fascia secondarily.
Neurologic changes (spasticity, weakness, altered movement patterns) can cause some muscles to over‑recruit while others under‑activate, leading toward fascial shortening, adhesions, and asymmetrical tension.
Reduced mobility and altered posture can create “imprinted” fascial patterns, where certain lines of the body become chronically tight or compressed, which may contribute to pain, reduced range of motion, and fatigue.
Fascial tightness can also compress nerves and vasculature, amplifying sensations of stiffness, burning, or band‑like discomfort during movement or stretching.
In MS, fascial work is best approached as supportive, not aggressive—gentle lengthening, rhythmic movement, and manual techniques that help restore balance without over‑stimulating a sensitive nervous system.
How stress, emotions, and mental health affect the fascia
Stress, emotions, and mental health have a profound “bottom‑up” effect on fascia because this tissue is densely laced with sensory nerves and deeply tied to the autonomic nervous system. When you’re under chronic stress or carrying unresolved grief, anxiety, or trauma, your body often responds with sustained muscle tension, altered breathing patterns, and protective postures, all of which can pull fascia into shortened, rigid patterns over time. These patterns not only feel like stiffness or “tightness” but can also compress nerves and blood vessels, leading to pain, fatigue, and a sense of being “stuck” physically and emotionally. On the other hand, practices that calm the nervous system—such as slow diaphragmatic breathing, gentle movement, mindfulness, and emotion‑aware bodywork—can help soften these fascial holding patterns, restoring glide, space, and a greater sense of embodied ease. From a holistic perspective, caring for mental and emotional health is not separate from fascial health; it’s an essential part of helping the body move, breathe, and heal with more fluidity.
Signs your fascia may be unhappy
When fascia is healthy, it’s pliable, well‑lubricated, and moves with ease. When it’s not, you may notice:
Tight bands or “knots” that feel like strings under the skin.
Limited range of motion, stiffness after sitting, or pain that feels vague or “deep” rather than localized.
Sensations that travel along lines (for example, shoulder‑to‑arm or low‑back‑to‑hip) because fascia connects regions across the body.
Tips to keep your fascia healthy
Because fascia is everywhere and responds directly to how you move, hydrate, and manage stress, small daily habits make a big difference. Here are practical, evidence‑informed tips you can easily weave into your wellness routine.
1. Move regularly and diversely
Fascia thrives on varied, moderate movement. Long periods of sitting or repetitive motions can cause fascia to bind and lose its glide. Aim for:
Daily walking, yoga, or slow stretching.
Changes in posture and position every 30–60 minutes, especially if you work at a desk.
2. Stretch gently and hold longer
Fascia responds best to slow, sustained holds that allow the gel‑like ground substance to shift. Try:
Holding stretches for at least 3–5 minutes, breathing deeply into the area.
Emphasizing full‑body lines (like a side‑body stretch or standing hamstring stretch) rather than isolated muscles.
3. Stay well‑hydrated and nourished
Because fascial ground substance is largely water and depends on nutrient‑rich building blocks, hydration and diet are non‑negotiable.
Drink water consistently throughout the day (an approximate guideline is half your body weight in ounces, adjusted for activity and climate).
Emphasize whole, anti‑inflammatory foods: vegetables, fruits, omega‑3 fats, lean proteins, and gut‑supportive fermented foods, while minimizing ultra‑processed sugars and fats.
4. Incorporate self‑myofascial release
Tools such as foam rollers, balls, or massage wands can gently unravel tight fascial layers and improve blood flow. When you use these:
Roll slowly and pause on tender spots for 20–30 seconds, letting the tissue soften.
Avoid rolling directly over bony joints or areas of acute injury without guidance.
5. Include hands‑on work and bodywork
Manual therapies like massage, myofascial release, and adaptive manual therapy can help normalize tension patterns and hydrate fascial layers.
For clients with EDS or hypermobility, prioritize gentle, proprioceptive touch and joint‑stabilizing strategies over aggressive stretching.
For clients with MS, focus on rhythmic, supportive patterns that ease spasticity lines and reduce neural irritation while preserving energy.
6. Prioritize recovery and load management
Acute or repetitive strain, along with poor recovery, can lead to inflammation and fascial stiffness. Support tissue health by:
Varying exercise intensity and avoiding excessive, repetitive motions.
Allowing rest and gentle movement days after heavier workouts or manual therapy sessions.
7. Honor the mind‑body connection
Fascia is richly innervated and responds to emotional and nervous‑system states; chronic stress and tension can show up as tight fascial patterns. Practices such as mindful breathing, meditation, gentle movement, and nervous‑system regulation can help soften both muscle and fascia from the inside out.




Comments